Gingivitis: A Common Oral Health Concern
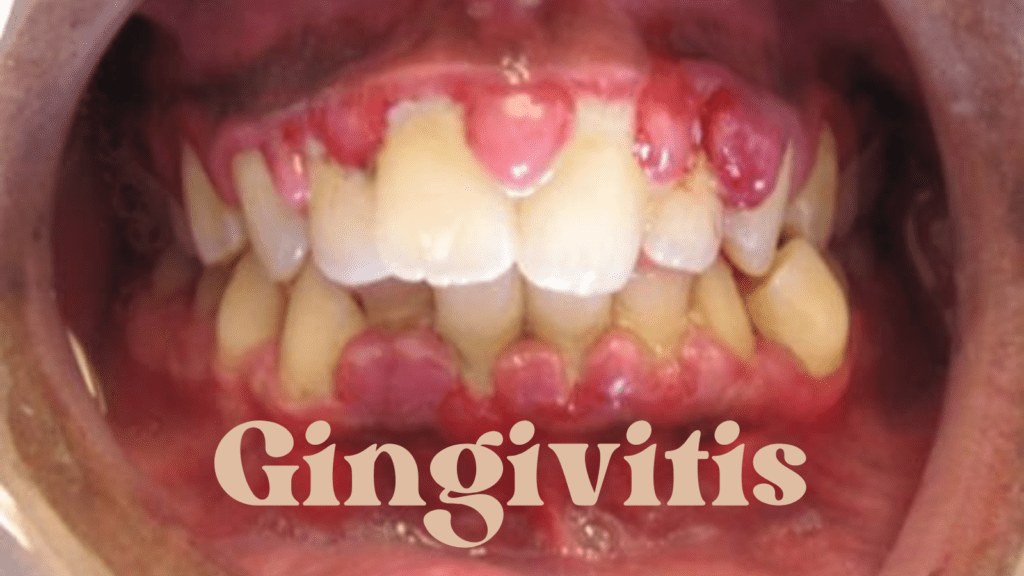
Gingivitis is a common and often underestimated oral health issue that affects millions of people worldwide. Although it may seem like a minor problem, untreated gingivitis can lead to more severe dental problems. In this blog post, we will explore the causes, symptoms, and prevention strategies for gingivitis to help you maintain a healthy smile.
What Is Gingivitis?
Gingivitis is the medical term for inflammation of the gums. It is often the initial stage of gum disease and is caused by the accumulation of plaque on your teeth. Plaque is a sticky, colorless film of bacteria that forms on your teeth when you don’t brush and floss regularly. If left untreated, gingivitis can progress to a more severe form of gum disease called periodontitis, which can lead to tooth loss and other complications.
Common Causes of Gingivitis
- Poor Oral Hygiene: Inadequate brushing and flossing habits are a significant factor. When you don’t brush and floss regularly, plaque builds up on your teeth and along the gumline, leading to inflammation and gingivitis.
- Inadequate Brushing Technique: Brushing too aggressively or using a toothbrush with hard bristles can damage the gums and make them more susceptible to gingivitis.
- Infrequent Dental Check-ups: Skipping regular dental check-ups and professional cleanings can allow gingivitis to go unnoticed and untreated.
- Smoking and Tobacco Use: Smoking and using tobacco products can compromise blood flow to the gums, making it easier for gingivitis to develop and more challenging to heal.
- Poor Nutrition: A diet lacking essential vitamins and minerals, particularly vitamin C, can weaken your immune system, making it less effective at fighting off infections like gingivitis.
- Stress: Chronic stress can compromise your immune system, making you more vulnerable to oral health problems like gingivitis.
- Medications: Some medications, such as certain antihypertensives and anticonvulsants, can lead to gum inflammation as a side effect.
- Hormonal Changes: Hormonal fluctuations during pregnancy, menstruation, and menopause can make the gums more susceptible to gingivitis.
- Medical Conditions: Certain medical conditions like diabetes, HIV/AIDS, cancer, and autoimmune diseases can increase your risk of developing gingivitis.
- Age: As you age, your risk of developing gingivitis increases. Older adults may have a higher likelihood of experiencing gum problems.
- Genetics: Some people may be genetically predisposed to developing gum disease, including gingivitis.
Common Symptoms of Gingivitis
Recognizing the signs of gingivitis is crucial for early intervention. Some common symptoms include:
- Red or Swollen Gums: Inflammation of the gum tissue often results in redness and puffiness. Healthy gums should appear pink and firm.
- Bleeding Gums: One of the hallmark signs of gingivitis is bleeding from the gums, especially when you brush or floss. This bleeding is often painless but can be an early warning sign.
- Bad Breath (Halitosis): Gingivitis can cause persistent bad breath due to the presence of bacteria in the mouth and the release of foul-smelling compounds.
- Tender or Painful Gums: Gingivitis can make your gums feel sensitive or sore, particularly when pressure is applied, such as when eating or brushing your teeth.
- Receding Gums: As gingivitis progresses, the gumline may start to recede, exposing more of the tooth’s surface and making the teeth appear longer than usual.
- Pus Between Teeth and Gums: In advanced cases of gingivitis, pockets can form between the teeth and gums, and these pockets may contain pus, which is a sign of infection.
- Changes in Your Bite: Gingivitis can lead to changes in the way your teeth fit together when you bite or chew. This can result from the loss of supporting gum and bone tissue.
It’s important to note that gingivitis is typically painless in its early stages, which can be deceiving. While you may not feel discomfort, the symptoms listed above are clear indicators of a problem with your gum health. Gingivitis can progress to a more severe form of gum disease called periodontitis, which can lead to tooth loss and other complications if left untreated.
Preventing Gingivitis
The good news is that gingivitis is largely preventable with proper oral hygiene and healthy lifestyle choices. Here are some tips to help you keep gingivitis at bay:
- Regular Brushing: Brush your teeth at least twice a day with fluoride toothpaste. Use a soft-bristle toothbrush, and be gentle to avoid damaging your gums. Brush for two minutes to ensure thorough cleaning.
- Floss Daily: Flossing is essential for removing plaque and food particles from between your teeth and along the gumline. Make it a daily habit to keep your gums healthy.
- Use an Antimicrobial Mouthwash: Rinse with an antimicrobial or fluoride mouthwash to reduce plaque and fight bacteria. Choose a mouthwash recommended by your dentist.
- Visit Your Dentist: Regular dental check-ups and cleanings are crucial for catching and treating gingivitis early. Your dentist can assess your oral health and provide professional cleaning to remove hardened plaque (tartar) that can’t be removed by regular brushing and flossing.
- Quit Smoking and Avoid Tobacco: Smoking and tobacco use can significantly increase your risk of developing gingivitis. Quitting these habits is beneficial for your overall oral health.
- Maintain a Balanced Diet: Consume a diet rich in fruits, vegetables, and whole grains. Limit sugary and acidic foods and beverages, as they contribute to plaque formation.
- Stay Hydrated: Drinking plenty of water helps rinse away food particles and bacteria, maintaining a cleaner mouth.
- Manage Stress: Chronic stress can weaken your immune system, making you more susceptible to gum problems. Practicing stress-reduction techniques, such as mindfulness or relaxation exercises, can help.
- Treat Medical Conditions: If you have medical conditions like diabetes or certain autoimmune diseases, work closely with your healthcare provider to manage them effectively. Well-controlled medical conditions can help lower your risk of gingivitis.
- Hormonal Awareness: Be aware of hormonal changes in your body, such as during pregnancy or menopause. These changes can affect gum health, so it’s essential to maintain good oral hygiene and consult with your dentist as needed.
- Genetic Factors: If gum disease runs in your family, be extra vigilant about your oral health and consider more frequent dental check-ups.
- Dental Appliances: If you wear dental appliances, such as braces or dentures, follow your dentist’s instructions for cleaning and care to prevent plaque buildup and gum irritation.
Remember that gingivitis is a largely preventable and manageable condition. By implementing these preventive measures and practicing good oral hygiene, you can reduce your risk of gingivitis and maintain healthy gums. If you suspect you have gingivitis or experience any symptoms, consult with a dentist for proper diagnosis and personalized treatment recommendations. Early intervention is key to preventing the progression of gum disease.
Disclaimer
The information provided in this blog post is for informational purposes only and should not be considered a substitute for professional medical or dental advice. Always consult with a qualified healthcare or dental professional for proper diagnosis, treatment, and guidance on your specific oral health needs.
Stay updated—subscribe now for informed empowerment!

